















Once you’ve got your plan management funding in place, you’re ready to start enjoying the benefits of life as a My Plan Manager client. It’s a quick, three-step process to join us, and then you’re on your way! It’s even quicker if you’re moving from another provider. Once you’re on board you can:
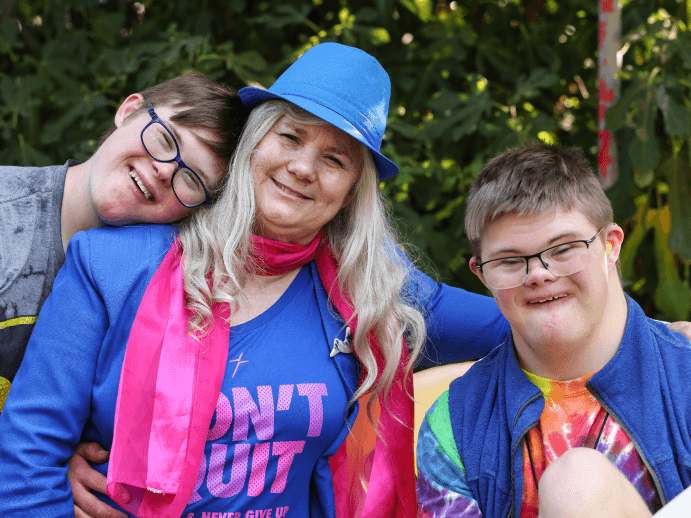
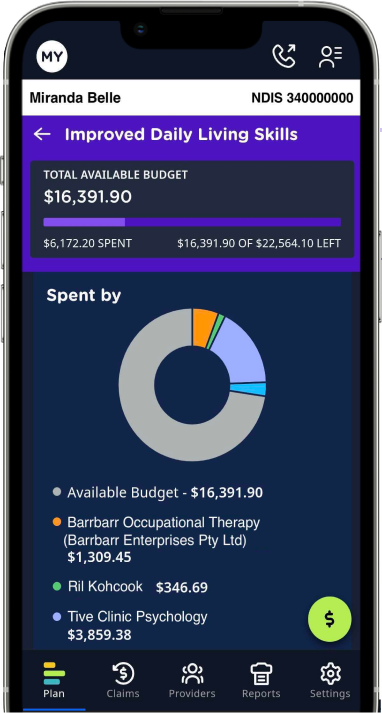







From the beginning of time, we’ve depended upon communities to provide us with connection and deliver the wellbeing benefits that come from it. So, we created one of our own for people with disability and their supporters, along with NDIS experts, disability sector professionals and service providers. That community is Kinora!
In Kinora, you can find more than 10,000 like-minded members with similar interests, experiences and challenges – and connect with providers and subject matter experts with the experience to help you get the most out of life. You may not know them, but inside Kinora’s moderated community you can swap advice and experiences and know you’re not alone.
And best of all, it’s a positive space, because it was built for one purpose only – to give and receive support – and that purpose has been honoured and carried into the Kinora culture from Day 1.
To learn more about the benefits Kinora offers, click here.









Clickability is a free provider directory listing providers that deliver a wide range of services across Australia. Start the search for your perfect provider today!


Say hello to My Plan Manager team members at the Hunter Disability Expo! The expo brings together pr...
May 10 - May 11
Chat with My Plan Manager team members at the Gold Coast Disability Expo! The expo brings together p...
June 7 - June 8